Understanding pleural effusions
Pleural effusions happen when too much fluid builds up in the space around the lungs. This extra fluid can press on the lungs and weigh down the diaphragm, making it hard to take a full breath.1,2
Pleural effusions can happen in people with cancer, heart or kidney failure, liver disease, or inflammatory conditions.1,2
Pleural effusions can cause1,2
- Shortness of breath
- Chest tightness or pressure
- Sharp pain when breathing in
- Persistent cough
- Fatigue
A vicious cycle

- Breathlessness
- Chest tightness
- Medical visit
- Fluid drainage
Hear how ACES™ has made breathing easier for people living with recurrent pleural effusions
Freedom from painful, repeat procedures
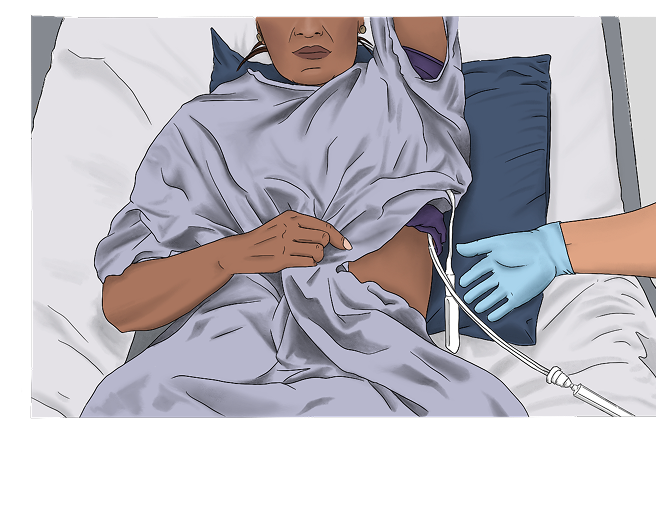
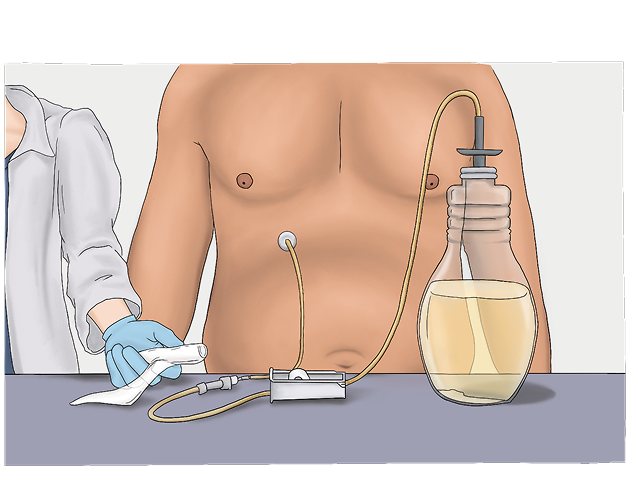
Indwelling pleural catheters (IPCs) are tubes placed in the chest with a small opening that stays outside the body so fluid can be drained at home.2,4
IPCs require frequent drainage using vacuum bottles and often needs support from home healthcare. It can also increase the risk of infection.2,4,5
Learn why ACES may be a better choice for managing pleural effusions
How does ACES Compare to other treatments for recurrent pleural effusions?
Typical treatments for chronic pleural effusions are pleurodesis and indwelling pleural catheters (IPCs). Pleurodesis is a procedure that uses a chemical to cause scarring and prevent fluid from building up in the pleural space.1 It can cover a permanent solution but is a painful procedure that requires a hospital stay.2 It is not appropriate for many patients. Indwelling Pleural Catheters (IPCs) are implanted catheters that have an externalized port to allow drainage of pleural effusions.3 This method requires regular drainage into single-use vacuum bottles, which often requires home healthcare assistance. IPCs have a high risk of infection and symptoms may return between drainage.4 The ACES device allows you to live your life more freely than other options. The ACES device is implanted in a short procedure with a brief hospital stay. There are no external catheters to drain or drainage bottles to manage and no restrictions on things like swimming or bathing.
1. Ali M, et al. Treasure Island (FL): StatPearls Publishing; 2025.
2. www.cancercenter.com/treatment-options/pleurodesis. 2025.
3. www.thoracic.org/ patients/patient-resources/resources/indwelling-tunneled-pleural-catheters. Patient Education | Information Series. 2025.
4. Lui, Complications of indwelling pleural catheter use and their management, BMJ 2015.
What is the procedure like and how long does it last?
The surgeon will make three incisions in the side of your chest, one for the pump and the others for the abdominal catheter. The implant procedure typically takes about an hour and is done under general anesthesia with a short hospital stay.
Is there much pain?
The pump incision may be tender for a few days. Some people have ongoing discomfort at the pump site that may require pain medication. Speak to your physician if you experience persistent pain.
What happens to the fluid that is pumped into my abdomen?
When the fluid from your chest is pumped into the abdomen, it is safely resorbed by the body.
Will I feel the device or will there be discomfort?
The ACES is a low-profile device that you will be able to feel under the skin so you can pump it if needed. It is implanted in an area that is typically not bothersome. Most patients do not report any discomfort.
What are the risks of ACES?
Risks include injury to lung, liver or bowel during implantation that can cause bleeding, air leaking out of your lung, or air and bacteria leaking out of your bowel. These would likely require additional treatment and a hospital stay. While the ACES is a low-maintenance option for patients, it is possible for the ACES to become clogged and stop working or become damaged; that fluid may again build up in your chest or begin to build up in your abdomen; that fluid may leak out of the incisions; that the incisions may become infected or that you could develop an infection in your chest or abdomen. Most of these issues can be easily resolved. Review the materials on caring for ACES carefully and contact your physician as directed.
Can I shower and swim?
Yes. Because ACES is fully internal, you can enjoy water activities once cleared by your doctor
This information is provided for educational purposes only and is not intended to replace the advice of your healthcare provider.
All medical procedures carry some risks and potential complications. Please discuss these in detail with your healthcare provider before making a decision.
References: 1. Shen-Wagner J, Gamble C, MacGilvray P. Pleural Effusion: Diagnostic Approach in Adults. Am Fam Physician. 2023 Nov;108(5):464-475. 2. American Thoracic Society. Indwelling tunneled pleural catheters (patient education information sheet). ATS Patient Information Series. 2019. Accessed December 8, 2025. https://craftprd1.blob.core.windows.net/documents/advocacy-patients/patient-resources/indwelling-tunneled-pleural-catheters.pdf craftprd1.blob.core.windows.net 3. Wright MJ, Nguyen PH, Backer ED, Goitein L, Feller-Kopman DJ. Recurrent malignant pleural effusion management: evaluating quality gaps, outcomes, costs, and adherence to guideline-consistent care. CHEST Pulmonary. 2025;(In press). 4. American Thoracic Society. Malignant pleural effusions (patient education fact sheet). ATS Patient Information Series. 2018. Accessed December 8, 2025. https://craftprd1.blob.core.windows.net/documents/advocacy-patients/patient-resources/malignant-pleural-effusions.pdf 5. Iyer NP, Reddy CB, Wahidi MM, Lewis SZ, et al. Indwelling pleural catheter versus pleurodesis for malignant pleural effusions. a systematic review and meta-analysis. Ann Am Thorac Soc. 2019 Jan;16(1):124-131.

